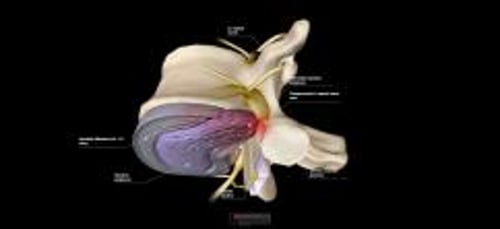
Herniated cervical disc is prolapse of the nucleus pulposus of the intervertebral disc through a tear in the surrounding annulus fibrosus. The tear causes pain due to irritation of sensory nerves in the disc, and when the disc impinges on an adjacent nerve root, a segmental radiculopathy with paresthesias and sometimes weakness in the distribution of the affected root results. Diagnosis is usually confirmed by MRI or CT. Treatment of mild cases is with analgesics, activity modification, and physical therapy. Patients with progressive or severe neurologic deficits, intractable pain, conservative treatment failure, or cervical myelopathy may require immediate or later elective surgery (eg, diskectomy, laminectomy).
Spinal vertebrae are separated by fibrocartilaginous discs consisting of an outer annulus fibrosus and an inner nucleus pulposus. When degenerative changes (with or without trauma) result in protrusion or rupture of the nucleus through the annulus fibrosus in the lumbosacral or cervical area, the nucleus is displaced posterolaterally or posteriorly into the extradural space.
Radiculopathy occurs when the herniated nucleus compresses or irritates the nerve root. Posterior protrusion may compress the cord in the cervical, thoracic, or upper lumbar spine or the cauda equina, especially in a congenitally narrow spinal canal (spinal stenosis). In the cervical spine, the C6 and C7 nerves are most commonly affected.
Herniated discs are common.
Symptoms and Signs of Cervical Disc Herniation
Herniated discs often cause no symptoms, or they may cause symptoms and signs in the distribution of affected nerve roots. Pain usually develops suddenly, and neck pain is typically relieved by rest and modification of activity. In contrast, nerve root pain caused by an epidural tumor or abscess begins more insidiously, and neck pain is often worse at night while in bed.
In patients with cervical disc herniations, there can be pain with flexion or combined extension and rotation, which can radiate to the upper extremities. Muscle weakness, numbness, and paresthesias can also be present in the upper extremities.
Diagnosis of Cervical Disc Herniation
MRI or CT
Diagnosis is usually suspected based on history and physical examination findings and confirmed by MRI or CT.
Physical examination should assess cervical spine movement and how it relates to the patient's symptoms. Neurological examination should include assessment of motor strength, sensation, and deep tendon reflexes. Passively extending the cervical spine, rotating the head to the side of the patient symptoms, and applying axial compression (Spurling or nerve compression test) may produce radicular pain in the upper extremity on the side to which the head is rotated.
MRI or CT can identify the cause and precise level of the lesion. Rarely (ie, when MRI is contraindicated and CT is inconclusive), CT myelography is necessary. Electrodiagnostic testing may help identify the involved root if the pain has been present for at least 4 weeks. Earlier testing may result in a false negative exam.
Because an asymptomatic herniated disc is common, the clinician must carefully correlate symptoms and findings on physical examination with MRI abnormalities before invasive procedures are considered.
Treatment of Cervical Disc Herniation
Conservative treatment initially
Invasive procedures, sometimes including surgery, if neurologic deficits are progressive or severe
Because a herniated disc desiccates and shrinks over time, symptoms tend to abate regardless of treatment. Approximately 75% of patients with acute cervical radiculopathy experience a significant reduction in pain without surgery within 6 weeks (1).
Conservative treatment
Treatment of a herniated disc should be conservative, unless neurologic deficits are progressive or severe. Heavy or vigorous physical activity is restricted, but ambulation and light activity (eg, lifting objects < 2.5 to 5 kg [about 5 to 10 lb] using correct techniques) are permitted as tolerated; prolonged bed rest (including traction) is not indicated.
Acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), or other analgesics should be used as needed to relieve pain. If symptoms are not relieved with nonopioid analgesics, corticosteroids are sometimes given systemically or as an epidural injection; however, their efficacy for cervical disc herniation is not well-established. Furthermore, analgesia tends to be modest and temporary at best. An example of an oral methylprednisolone tapering regimen that may be used starts with 24 mg daily and is decreased by 4 mg a day, to be completed over 6 days.Acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), or other analgesics should be used as needed to relieve pain. If symptoms are not relieved with nonopioid analgesics, corticosteroids are sometimes given systemically or as an epidural injection; however, their efficacy for cervical disc herniation is not well-established. Furthermore, analgesia tends to be modest and temporary at best. An example of an oral methylprednisolone tapering regimen that may be used starts with 24 mg daily and is decreased by 4 mg a day, to be completed over 6 days.
In selected patients, gabapentin and amitriptyline are used for refractory neuropathic pain.In selected patients, gabapentin and amitriptyline are used for refractory neuropathic pain.
Physical therapy and home exercises can improve posture and strengthen neck muscles and thus reduce spinal movements that further irritate or compress the nerve root.
Surgical procedures
Surgical procedures should be considered for the following:
Persistent or worsening neurologic deficits, particularly objective deficits (eg, weakness, reflex deficits) due to cervical radiculopathies
Acute compression of the spinal cord, causing myelopathy
Severe, intractable nerve root pain or sensory deficits
Immediate surgical evaluation is needed if clinical findings of spinal cord compression correlate with MRI abnormalities.
Anterior diskectomy and cervical fusion are the most common treatments for cervical radiculopathies. Laminectomies are not performed alone without posterior fusion due to the complication of cervical kyphosis.
Dissolving herniated disc material with local injections of the enzyme chymopapain is not recommended.
Lesions acutely compressing the spinal cord causing myelopathy require immediate surgical evaluation (see diagnosis of spinal cord compression).
If cervical radiculopathies are accompanied by signs of spinal cord compression, surgical decompression is needed immediately; otherwise, it is done electively when nonsurgical treatments are ineffective.
Treatment reference
1. Beckworth WJ, Abramoff BA, Bailey IM, et al. Acute Cervical Radiculopathy Outcomes: Soft Disc Herniations vs Osteophytes. Pain Med. 2021;22(3):561-566. doi:10.1093/pm/pnaa341
Key Points
Cervical herniated discs are common and most commonly affect nerve roots at C6 and C7.
If symptoms develop suddenly and neck pain is relieved with rest, suspect a herniated disc.
Diagnose based on history and physical examination findings, and confirm by MRI or CT.
Recommend analgesics, light activity as tolerated, and exercises to improve posture and strength; however, if pain or deficits are severe or worsening, consider surgical procedures.
Drug Information for the Topic