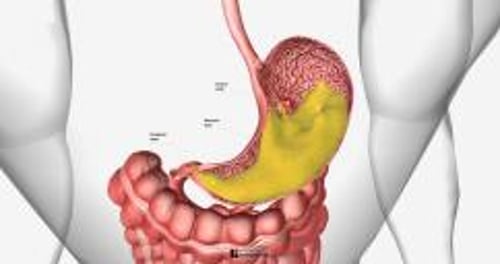
A peptic ulcer is a round or oval sore where the lining of the stomach or duodenum has been eaten away by stomach acid and digestive juices.
Peptic ulcers can result from infection with Helicobacter pylori bacteria or from use of medications, such as aspirin or other nonsteroidal anti-inflammatory drugs (NSAIDs), that weaken the lining of the stomach or duodenum.
Discomfort caused by ulcers comes and goes and tends to be related to meals (sometimes better after eating and sometimes worse after eating).
The diagnosis of peptic ulcer disease is based on symptoms of stomach pain and on the results of an examination of the stomach with a flexible viewing tube (upper endoscopy) and of Helicobacter pylori testing.
Medications are given to reduce acid in the stomach, and antibiotics often are given to eliminate Helicobacter pylori.
(See also Introduction to Gastritis and Peptic Ulcer Disease.)
Ulcers penetrate into the lining of the stomach or duodenum (the first part of the small intestine). Ulcers may range in size from several millimeters to several centimeters.
Ulcers can occur at any age, including infancy and childhood, but are most common among middle-aged adults.
Gastritis (stomach inflammation) may develop into ulcer disease.
The names given to specific ulcers identify their anatomic locations or the circumstances under which they developed.
Duodenal ulcers, the most common type of peptic ulcer, occur in the first few inches of the small intestine (called the duodenum).
Gastric ulcers (stomach ulcers) are less common and usually occur in the lower part of the stomach.
This photo shows a large ulcer (arrow) in the stomach.
Marginal ulcers can develop when part of the stomach has been removed surgically, at the point where the remaining stomach has been reconnected to the intestine.
Stress ulcers, like those that form in acute stress gastritis, can occur as a result of the stress of severe illness, skin burns, or injury. Stress ulcers occur in the stomach and the duodenum.
Causes of Peptic Ulcer Disease
Ulcers develop when the normal defense and repair mechanisms of the lining of the stomach or duodenum are weakened, making the lining more likely to be damaged by stomach acid.
By far, the 2 most common causes of peptic ulcers are
Helicobacter pylori infection of the stomach
Use of nonsteroidal anti-inflammatory drugs (NSAIDs), such as aspirin, ibuprofen, or naproxen(NSAIDs), such as aspirin, ibuprofen, or naproxen
H. pylori infection is present in more than 50% of people with duodenal ulcers and in 30 to 50% of people with stomach ulcers.
NSAID use causes more than 50% of peptic ulcers. However, most people who take NSAIDs do not develop peptic ulcers.
People who smoke are more likely to develop a peptic ulcer than people who do not smoke, and their ulcers heal more slowly and are likely to return.
Although alcohol increases stomach acid production, drinking moderate amounts of alcohol does not seem to cause ulcers or delay their healing.
A rare cause of peptic ulcers is a type of cancer that releases a hormone called gastrin that causes excess acid production (see Zollinger-Ellison Syndrome). The symptoms of cancerous ulcers are very similar to those of noncancerous ulcers. However, cancerous ulcers usually do not respond well to the treatments used for noncancerous ulcers.
About 50 to 60% of children who have duodenal ulcers have a family history of peptic ulcer disease.
Symptoms of Peptic Ulcer Disease
Symptoms of peptic ulcer disease can vary with the location of the ulcer and the person's age. For example, children, older adults, and people whose ulcers were caused by NSAIDs may not have the usual symptoms or may have no symptoms at all. In these instances, ulcers are discovered only when complications develop.
The most common symptom of a peptic ulcer is
Mild to moderately severe pain in the upper abdomen
The pain is typically described as gnawing, burning, aching, or soreness or sometimes as a sensation of hunger and is usually located in the upper abdomen just below the breastbone. It is usually relieved by food or antacids. The typical ulcer tends to heal and return. Thus, pain may occur for days or weeks, then wane or disappear, and then return again when the ulcer returns. Only about half of people have typical symptoms.
Duodenal ulcer symptoms tend to follow a pattern. People usually do not have pain when they awaken, but pain appears by mid-morning. Drinking milk or eating (which buffers stomach acid) or taking antacids generally relieves the pain, but it usually returns 2 or 3 hours later. Pain that awakens the person during the night is common. Frequently, the pain occurs one or more times a day over a period of one to several weeks and then may go away without treatment. However, pain usually returns, often within the first 2 years and occasionally after several years. People generally develop patterns and often learn by experience when a recurrence is likely (commonly in spring and fall and during periods of stress).
The symptoms of gastric ulcers, marginal ulcers, and stress ulcers, unlike those of duodenal ulcers, do not follow any pattern. Eating may relieve pain temporarily or may cause pain rather than relieve it. Gastric ulcers sometimes cause scarring and swelling of the tissues (edema) that lead into the small intestine, which may prevent food from easily passing out of the stomach. This blockage may cause bloating, nausea, or vomiting after eating.
Complications of Peptic Ulcer Disease
Most peptic ulcers can be cured without complications. However, in some cases, peptic ulcers can develop potentially life-threatening complications, such as
Bleeding (hemorrhage)
Penetration
Perforation
Obstruction (blockage)
Cancer
Bleeding
Bleeding (hemorrhage) is the most common complication of ulcers even when they are not painful (see Gastrointestinal Bleeding). Vomiting bright red blood or reddish brown clumps of partially digested blood that look like coffee grounds (hematemesis) and passing black tarry stools (melena) or obviously bloody stools (hematochezia) can be symptoms of a bleeding ulcer. Small amounts of blood in the stool may not be noticeable but, if persistent, can still lead to anemia. Blood loss may also cause weakness, a decrease in blood pressure when a person stands up, sweating, thirst, and fainting.
Bleeding may result from other digestive conditions as well, but doctors begin their investigation by looking for the source of bleeding in the stomach and duodenum. Unless bleeding is massive, a doctor uses a flexible viewing tube (endoscope) to do an upper endoscopy. If a bleeding ulcer is seen, the endoscope can be used to cauterize it (that is, stop the bleeding with heat). A doctor may also use the endoscope to inject a material that causes a bleeding ulcer to clot.
If the source cannot be found and the bleeding is not severe, treatments include taking medications that suppress the production of acid, such as histamine-2 (H2) blockers or proton pump inhibitors. The person also often receives fluids by vein and takes nothing by mouth, so the digestive tract can rest. If these measures fail, surgery may be needed.
Penetration
An ulcer can go through (penetrate) the muscular wall of the stomach or duodenum (the first segment of the small intestine) and continue into an adjacent organ, such as the liver or pancreas. This penetration causes intense, piercing, persistent pain, which may be felt in another area of the body other than the area involved. For example, the back may hurt when a duodenal ulcer penetrates the pancreas. The pain may intensify when the person changes position.
Doctors use imaging tests such as computed tomography (CT) and magnetic resonance imaging (MRI) to diagnose penetrations.
If medications do not heal the ulcer, surgery may be needed.
Perforation
Ulcers on the front surface of the duodenum or, less commonly, the stomach, can go through the wall, creating an opening (perforation) to the free space in the abdominal cavity. The resulting pain is sudden, intense, and steady. The pain rapidly spreads throughout the abdomen. The person may feel pain in one or both shoulders. Breathing deeply and changing position worsen the pain, so the person often tries to lie very still. The abdomen is tender when touched, and the tenderness worsens if a doctor presses deeply and then suddenly releases the pressure. (Doctors call this rebound tenderness.)
Symptoms of perforation may be less intense in older adults, in people taking corticosteroids or immunosuppressants, or in very ill people. A fever indicates an infection in the abdominal cavity. If the condition is not treated, shock may develop.
Doctors do x-rays or CT to aid the diagnosis.
This emergency situation (called an acute abdomen) requires immediate surgery and antibiotics given by vein.
Obstruction
Swelling of inflamed tissues around an ulcer or scarring from previous ulcer flare-ups can narrow the outlet from the stomach or narrow the duodenum. A person with this type of obstruction may vomit repeatedly—often regurgitating large volumes of food eaten hours earlier. A feeling of being unusually full after eating, bloating, and a lack of appetite are symptoms of obstruction. Over time, vomiting can cause weight loss, dehydration, and an imbalance in body chemicals (electrolytes).
Doctors base the diagnosis of obstruction on the results of x-rays.
Treating the ulcer and swelling with medications relieves the obstruction in most cases, but severe obstructions caused by scarring may require endoscopic dilation or surgery.
Cancer
People with ulcers caused by Helicobacter pylori are 3 to 6 times more likely to develop stomach cancer later in life. There is no increased risk of developing cancer from ulcers that have other causes.
Diagnosis of Peptic Ulcer Disease
Upper endoscopy
A doctor suspects an ulcer when a person has characteristic stomach pain. Sometimes the doctor simply treats the person for an ulcer to see whether the symptoms resolve (called empiric therapy). If the symptoms resolve, the person most likely had an ulcer.
Tests may be needed to confirm the diagnosis, especially when symptoms do not resolve after a few weeks of treatment, or when they first appear in a person who is over age 60 years or who has other symptoms such as weight loss, because stomach cancer can cause similar symptoms. Also, when severe ulcers resist treatment, particularly if a person has several ulcers or the ulcers are in unusual places, a doctor may suspect an underlying condition that causes the stomach to overproduce acid.
To help diagnose ulcers and determine their cause, the doctor does upper endoscopy (a procedure done using a flexible viewing tube called an endoscope).
During endoscopy, a doctor can do a biopsy (removal of a tissue sample for examination under a microscope) to determine if a gastric ulcer is cancerous and to help identify the presence of Helicobacter pylori bacteria. An endoscope also can be used to stop active bleeding and decrease the likelihood of recurring bleeding from an ulcer.
Blood tests to measure gastrin levels are done in people who may have Zollinger-Ellison syndrome.
Treatment of Peptic Ulcer Disease
Antibiotics
Acid-reducing medications
Antacids
Sometimes surgery
Because infection with H. pylori bacteria is a major cause of ulcers, treatment of H. pylori infection with 2 antibiotics together with bismuth subsalicylate and a proton pump inhibitor (called quadruple therapy) is given when infection is diagnosed. Several different antibiotics may be used, including amoxicillin, clarithromycin, metronidazole, and tetracycline. Some treatments include 2 antibiotics and a proton pump inhibitor without infection with 2 antibiotics together with bismuth subsalicylate and a proton pump inhibitor (called quadruple therapy) is given when infection is diagnosed. Several different antibiotics may be used, including amoxicillin, clarithromycin, metronidazole, and tetracycline. Some treatments include 2 antibiotics and a proton pump inhibitor withoutbismuth subsalicylate (called triple therapy).
Acid-reducing medications block the production of stomach acid. The most commonly used acid-reducing medications include proton pump inhibitors and histamine-2 (H2) blockers (see also Medications for the Treatment of Stomach Acid). Proton pump inhibitors promote healing of ulcers in a greater percentage of people in a shorter period of time than do H2 blockers and thus are typically preferred to H2 blockers for treating ulcers.
Antacids, such as liquids or tablets that contain calcium carbonate or similar substances, neutralize stomach acid but do not block its production.such as liquids or tablets that contain calcium carbonate or similar substances, neutralize stomach acid but do not block its production.
Neutralizing or reducing stomach acid promotes healing of peptic ulcers regardless of the cause. In most people, treatment is continued for 4 to 8 weeks. Although bland diets may help reduce acid, no evidence supports the belief that such diets speed healing or keep ulcers from recurring. Nevertheless, it makes sense for people to avoid foods that seem to make pain and bloating worse. Eliminating possible stomach irritants, such as NSAIDs, alcohol, and nicotine, is also important.
Surgery for ulcers is rarely needed because medications so effectively heal peptic ulcers and endoscopy so effectively stops active bleeding. Surgery is used primarily to deal with complications of a peptic ulcer, such as
A perforation
An obstruction that fails to respond to medication or that recurs
Two or more major episodes of bleeding ulcers
A gastric ulcer suspected of being cancerous
Severe and frequent recurrences of peptic ulcers
A number of different surgical procedures may be done to treat these complications. Surgery can also be done to reduce the production of acid and ensure the stomach can drain properly. However, ulcers may recur after surgery, and each procedure may cause problems of its own, such as weight loss, poor digestion, frequent bowel movements (dumping syndrome), and anemia.
Prognosis for Peptic Ulcer Disease
If Helicobacter pylori infection is successfully treated, peptic ulcer disease comes back in only 10% of people. However, peptic ulcer disease comes back in 50% of infected people when Helicobacter pylori infection is not eradicated.